- Home
-
SERVICES
Services offered by RM
-
SPECIALITIES
Major specialities
- WHY RM?
- SOFTWARES
- COMPLIANCES
- ABOUT US
Please fill out the form below if you have a plan or project in mind that you'd like to share with us.
Happy Clients
Projects Delivered
Skilled Employees
Support Available
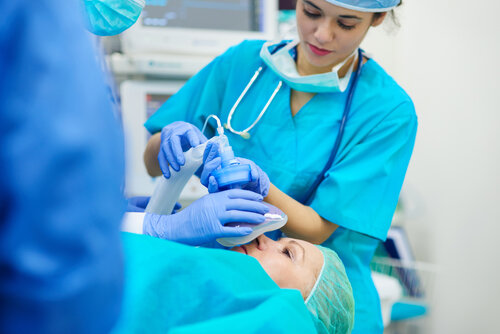
Anesthesiology deals with the total perioperative care of patients before, during, and after surgery. The specialty's core element is the use of anesthesia and anesthetics to support the vital functions through the perioperative period safely.
An anesthesiologist administers the right dosage of drugs to the patient so that’s he/she does not feel any pain or regain consciousness during surgery. They are also responsible for waking the patient post-surgery. They monitor the patient’s vitals keenly during surgery and alter the dosage administered accordingly.
There are different levels of Anesthesia providers - the Anesthesiologists, Certified Registered Nurse Anesthetists (CRNA), and Anesthesiologist Assistants (AA). They take on a critical role in understanding the patient’s history & conditions. But unfortunately, they are justified that they get billed correctly for their Services and get reimbursement to the maximum.
Anesthesia billing can become complicated as it requires documentation of a high number of records, such as:
The Anesthesia sheet involves the documentation of the following:
Base Units : The base units reflect the complexity and the skills required for the anesthetic service provided. The CMS publishes the base units once every year.
Time Units : This is the time spent with the patient administering the anesthetic or monitoring the patient’s condition before, after, or during the surgery. Time units are calculated by dividing the total minutes of service by 15
Modifiers : Anesthesia “provision/supervision” modifiers (-AA, -QK, -QY, -QZ, and -QX) explain the role of the anesthesiologist and CRNA. These modifiers are essential for clarifying whether an anesthesia procedure was personally performed, medically directed, or medically supervised by an anesthesiologist.
Formula : (Base Units + Time Units + Modifiers) x Conversion Factor = Anesthesia Reimbursement
Bundled Services : (Base Units + Time Units + Modifiers) x Conversion Factor = Anesthesia Reimbursement
Post-operative Review. The post-operative review consists of records that state that the patient has not suffered any complications due to the anesthetic administered.
The success of an anesthesiology service largely depends on its ability to generate & collect revenue. The ingredients for successful anesthesia billing include an experienced and trained revenue cycle team, specialty-specific billing software, and compliant billing practices. Outsourcing your billing & coding needs will help shift your focus to offering improved patient care. RM Healthcare consists of a team of experts who receive specialized training in billing for anesthesiology Services.
At RM Healthcare, we have a client base that extends over 50 states covering a wide range of hospitals, physician practices, and medical billing companies. Our coders are proficient in ICD-9/10, CPT, HCPCS codes based on CMS and AMA guidelines and certified by the American Academy of Professional Coders (AAPC). It would be fair to state that we have a decade of experience in pediatric billing & coding.
By obtaining authorization and validating the patient's eligibility and benefits before the surgery. We are also aware of the Services that can or cannot be bundled together with the anesthesiology service offered. In case of the absence of a valid medical reason for the necessity of a drug administered, we follow-up with the physician, clarify the medical necessity for the procedure, and state it clearly to claim rejection. Our expertise in Anesthesiology billing & coding includes but is not limited to:
We bring nothing less than excellence, knowledge, and accuracy while building a revenue cycle devoid of defects for your practice. Our team strives to introduce a friction-free billing, coding, claim submission, and payment posting process. To help achieve maximum reimbursements, we ensure that.
We bring nothing less than excellence, knowledge, and accuracy while building a revenue cycle devoid of defects for your practice. Our team strives to introduce a friction-free billing, coding, claim submission, and payment posting process. To help achieve maximum reimbursements, we ensure that.
















