- Home
-
SERVICES
Services offered by RM
-
SPECIALITIES
Major specialities
- WHY RM?
- SOFTWARES
- COMPLIANCES
- ABOUT US
Please fill out the form below if you have a plan or project in mind that you'd like to share with us.
Happy Clients
Projects Delivered
Skilled Employees
Support Available
The practice of applying universal alphanumeric codes to the many aspects of healthcare that have been provided, such as medical diagnosis, procedures, Services, and equipment provided, is referred to as medical coding. When assigning diagnostic and treatment codes to a patient, a medical coder will use the patient's medical record, which includes documents such as a physician's notes, laboratory reports, and service lists, as their primary source. The process of medical coding begins with the abstraction of medical information from the documentation that is readily available, continues with the assignment of the appropriate diagnosis and procedure codes, and concludes with the facilitation of the process of creating a claim that can be sent to payers.
It is essential to have medical coding of a high quality in order to receive appropriate reimbursements. Errors in medical coding can be expensive and lead to claim denials. Furthermore, they can create unjustified compliance difficulties, which can be even more costly.
Medical coders at RM Healthcare hold credentials from both the American Academy of Professional Coders (AAPC) and the American Health Information Management Association (AHIMA). Our staff is able to assure the greatest level of accuracy in medical coding because we have qualifications such as CPC (Certified Professional Coders) and its variants such as CPC-H/CPC-I) and CCS (Certified Coding Specialist).
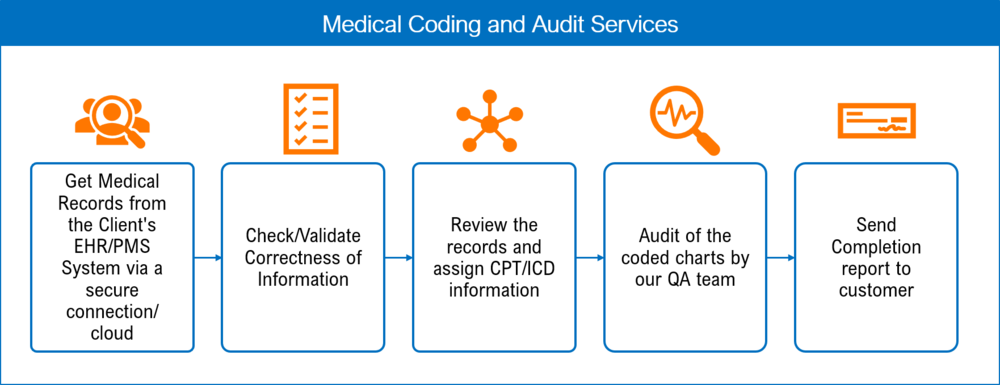
RM Healthcare provides the following medical coding Services:
Our medical coders follow the procedures outlined by our clients in their extensive work instructions and code based on the relevant clinical material. Coding for medical procedures is carried out in accordance with the procedures outlined by our clients in exhaustive work instructions, using only the most up-to-date clinical documentation. An experienced and certified coding auditor reviews the work of medical coders to ensure accuracy and compliance with industry standards. We promise the fastest turnaround times and highest standards of coding accuracy in the business.
Our clients regularly ask us to conduct a medical billing audit of the coding done by their staff in the United States, in addition to auditing all the coding work given to us. Using their expertise, our medical billing auditors ensure that all processes are being followed to the letter and that no coding mistakes are being made.
Our coding team also performs coding-related denial analysis, code corrections and resubmits the claims back to payers to improve reimbursements.
We have a very comprehensive coding training process. Each coder deployed on the customer account is thoroughly trained and goes through ongoing refresher training.
Our Coding training process includes:
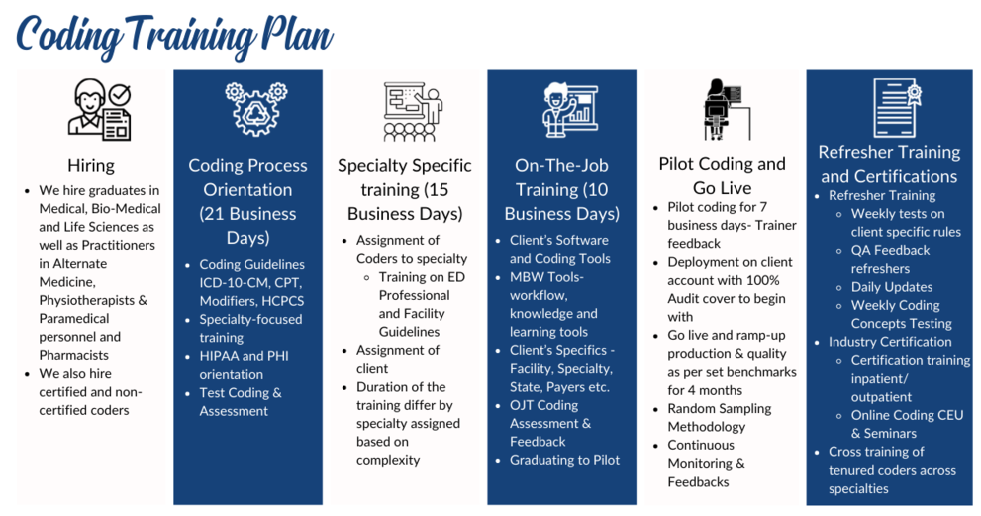
Did you know that medical practices bleed as much as 15% of their annual revenue due to errors in medical coding processes or on account of Discharges not Fully Billed? RM Healthcare coding team to run your coding processes efficiently and effectively.
Our coding team provides you the following benefits:
















