- Home
-
SERVICES
Services offered by RM
-
SPECIALITIES
Major specialities
- WHY RM?
- SOFTWARES
- COMPLIANCES
- ABOUT US
Please fill out the form below if you have a plan or project in mind that you'd like to share with us.
Happy Clients
Projects Delivered
Skilled Employees
Support Available
The efficiency of your revenue cycle can be gauged, in part, by how quickly and accurately payments are posted. You can analyze reimbursement patterns and trends with this information. Because timely and accurate payment posting is essential for understanding the health of your revenue cycle, it is important to hire a competent staff to handle this task.
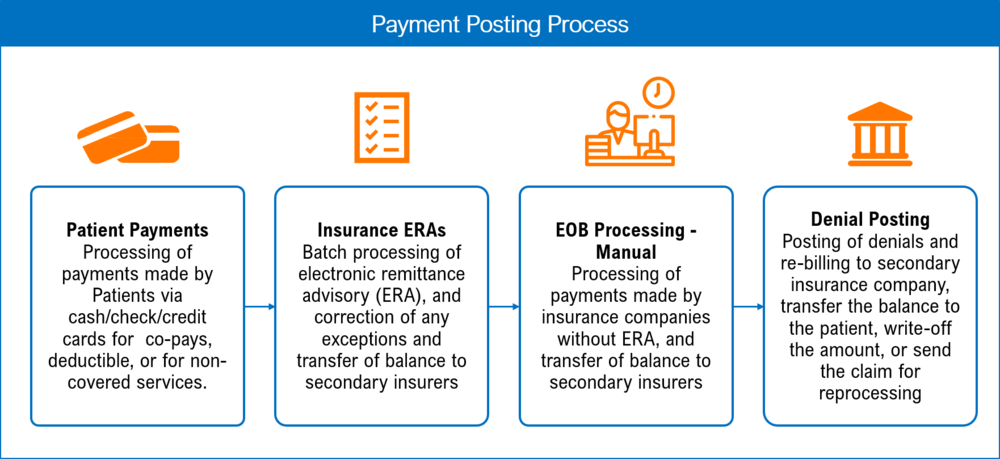
We process different types of remittances received with a high degree of accuracy, improved responsiveness, and follow the procedures defined by our clients. We perform the following Services:
Patient Payments : Our clients report patient payments made at the time of service to us. Co-payments, deductibles, and payments for uninsured services are all examples of what these payments are used for. After reviewing the data, our team makes the necessary adjustments to each patient's account.
Insurance Posting : We process Insurance Payments in the following formats
Insurance Payment Posting – Manual : Despite the prevalence of electronic EOBs provided by many payers, manual EOBs are still occasionally sent alongside payments. In accordance with the regulations for adjustments, write-offs, and balance transfers that we have established along with each facility/practice, the RM Healthcare team handles these payments with a high degree of precision.
Insurance Payment Posting – Electronic (ERA) — At the time of service, our clients inform us that patients have paid for their care. These are used for things like deductibles, co-pays, and out-of-pocket costs for services that aren't covered by insurance. Our team reviews the information and makes the required changes to each patient's account.
Denial Posting — Posting denied claims is crucial for gaining an accurate picture of the A/R cycle for each customer. When a claim is denied, the payer will often send back an ANSI rejection code and, in certain cases, medical coding instructions that are unique to that payer. We are well-versed in both ANSI standard denial codes and the codes used by most major payers. If a claim is denied, we document it in our practice management system and either resubmit it to the original insurer, bill the patient directly, cancel the claim, or resubmit it for reprocessing.
High Quality : We have a contractual guarantee of over 97% accuracy with our international delivery staff, but in practice we achieve over 99% accuracy.
Responsiveness : Our team is available 24/7, so we can promise a response within 1 business day.
Get an accurate understanding of the A/R cycle : For an accurate picture of your accounts receivable and thus the ability to make sound judgements, it is essential that payments be posted accurately.
Analytics : We generate reports on A/R trends to:
Exception processing : We adhere to your company policies and let you know about any major changes, contractual amendments, or denials.
















