- Home
-
SERVICES
Services offered by RM
-
SPECIALITIES
Major specialities
- WHY RM?
- SOFTWARES
- COMPLIANCES
- ABOUT US
Please fill out the form below if you have a plan or project in mind that you'd like to share with us.
Happy Clients
Projects Delivered
Skilled Employees
Support Available
We have a firm grasp of the regulations governing Medical Billing Services and payers, and we employ technological means to verify that these regulations are followed. Quick turnaround from the coders to transmission is guaranteed by our claims entry and transmission staff. Claims generation and transmission only take a few hours post-coding for clients where we have been able to deploy automated systems and Bots.
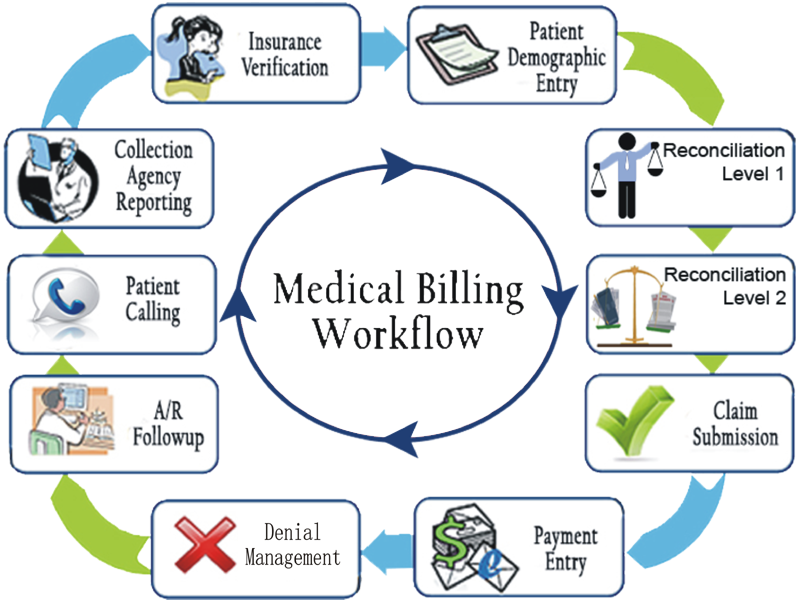
To create claims, we either manually enter costs or use electronic medical record interfaces to retrieve coded charts. To the client's PMS, we push charges that we've entered in our own systems.
To avoid delays in processing claims, we deploy workers at different times throughout the day as part of our medical billing services. To ensure minimal payment delays, clearing agency professionals work around the clock to monitor rejections and clear modifications through the payer portals.
RM Healthcare's automated system means there is no longer any need for human involvement in the charge input process. Our BOTs have built-in modifications that will scrub the claim to capture any inaccuracies on the claim form even before transmission, saving you time in addition to the obvious benefits.
















